Acute Laryngitis in Children: What Parents Need to Know
An early spring morning. In little Tolik’s family, nothing foretold trouble. The night before, he went to bed with a slight runny nose, and his mother simply thought, “He must be catching a cold.”
But before dawn, Tolik woke up with a loud, “barking” cough and a whistling sound on inhalation. His eyes were full of fear, his breathing labored, and the skin around his neck pulled in with every breath. His mother quickly sat him up, hugged him, and carried him into a steamy bathroom to breathe in moist air. Within a few minutes, his breathing became calmer, but his voice remained hoarse.
His mother immediately sought help from an ENT doctor. The diagnosis — croup. The ENT prescribed treatment and warned: the attack might return at night, and action must be taken without delay.
What would you do if such a situation happened in your family?
Introduction
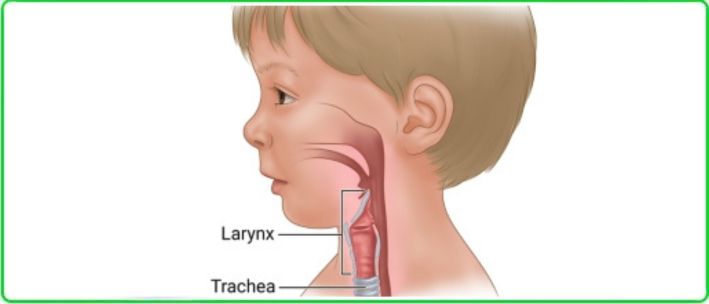
Acute laryngitis is an inflammation of the laryngeal mucosa that, in children, can rapidly progress to a life-threatening condition – airway narrowing (laryngeal stenosis). This happens because a child’s airway is significantly narrower than that of an adult, and the mucosa is looser and more prone to swelling. A viral infection that might cause only hoarseness in an adult can, in a child, lead to severe breathing difficulties.
Causes of Acute Laryngitis in Children
In approximately 90% of cases, acute laryngitis is caused by viral infections, including:
- Parainfluenza virus (most common)
- Respiratory syncytial virus (RSV)
- Influenza viruses
- Adenoviruses
Less commonly, bacterial pathogens such as Streptococcus or Staphylococcus aureus are responsible, or the condition may result from allergic reactions.
Risk factors include:
- Hypothermia and exposure to cold air
- Inhalation of dry indoor air
- Close contact with infected individuals
- Decreased immunity
Clinical Presentation
Typical symptoms include:
- Harsh, “barking” dry cough
- Hoarseness or aphonia (loss of voice)
- Noisy, labored breathing (stridor)
- Fever (normal to 39–40°C / 102–104°F)
- Runny nose, sore throat, irritability or lethargy
A particularly dangerous form is acute obstructive laryngotracheitis, also known as viral croup.
Signs of severe airway involvement (croup):
- Stridor even at rest
- Retraction of intercostal spaces during inspiration
- Pallor or cyanosis of the lips and skin
This is a medical emergency requiring immediate intervention.
Staging of Laryngeal Stenosis
Doctors classify airway narrowing into four stages:
- Compensation – mild stridor only during crying.
- Partial compensation – stridor at rest, moderate cyanosis.
- Decompensation – pronounced cyanosis, severe dyspnea, agitation or lethargy.
- Asphyxia – critical condition with loss of consciousness.
First Aid Before Medical Consultation
If your child shows signs of acute laryngitis or croup:
- Keep your child calm – crying worsens swelling.
- Ensure cool, humidified air (open a window, use a humidifier).
- Hold the child upright in your arms.
- If fever exceeds 38.5°C (101.3°F), give an age-appropriate antipyretic (paracetamol or ibuprofen).
- Avoid throat sprays in children under 3 years — they may trigger laryngeal spasm.
Diagnosis and Laryngoscopy
In addition to history and physical examination, the ENT specialist may perform laryngoscopy to directly visualize the larynx.
Findings in acute laryngitis:
- Redness and swelling of the vocal folds
- Subglottic edema
- Narrowing of the airway lumen
- Mucous or mucopurulent secretions
Purpose of laryngoscopy:
- Exclude other dangerous conditions (epiglottitis, foreign body, papillomatosis)
- Assess the degree of stenosis
- Guide treatment decisions
Flexible fiberoptic laryngoscopy, often performed through the nose, is quick (1–2 minutes) and allows dynamic assessment of the airway while maintaining spontaneous breathing.
Treatment Approaches
Mild cases:
- Budesonide via nebulizer
- Voice rest, cool humidified air
- Observation and hydration
Moderate severity:
- Budesonide + systemic corticosteroid (dexamethasone or prednisolone) if no improvement after inhalation therapy
Severe cases:
- High-dose corticosteroids
- Oxygen therapy
- Airway support (possible intubation in advanced stages)
- Antibiotics only for bacterial superinfection (e.g., cefuroxime, ceftriaxone)
Continuous monitoring is essential, with reassessment every 30–60 minutes in hospital settings.
Prevention
- Maintain optimal indoor humidity (40–60%)
- Avoid contact with sick individuals during viral outbreaks
- Annual influenza vaccination
- Timely treatment of nasal and throat infections
- Strengthening the immune system through balanced nutrition and outdoor activity
Doctor’s Advice
“At the first sign of breathing difficulty in your child, do not wait — contact an ENT specialist immediately. Acute laryngitis in children can deteriorate quickly, but timely medical intervention can save a life.”
— Dr. Maryna Kryshtopava, PhD, Associate Professor, ENT Specialist












